Mitralklappeninsuffizienz (MI) macht die überwiegende Mehrheit aller Mitralklappenerkrankungen aus.1 Sie hat eine Prävalenz von etwa 2 % in der Allgemeinbevölkerung und tritt häufiger bei älteren Menschen auf.3 Etwa 10 % der Menschen über 70 sind von einer klinisch bedeutsamen MI betroffen.5
Unbehandelt kann MI zu Herzinsuffizienz (HI) oder einer Verschlechterung einer bereits bestehenden Herzinsuffizienz führen, was zu einer erhöhten Zahl von Hospitalisierungen und einer erheblichen Kostenbelastung für die Gesundheitssysteme führt.6,8
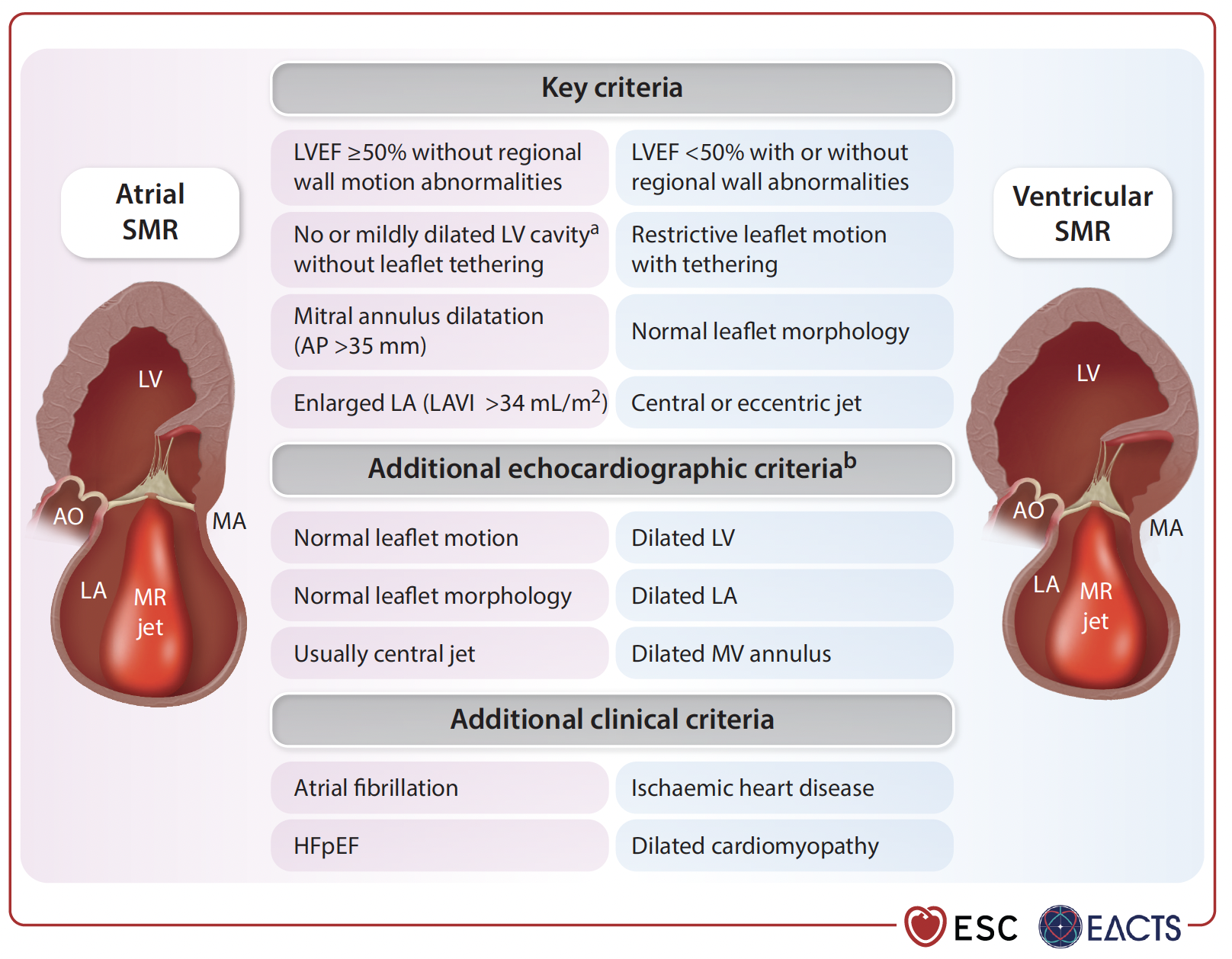
TEER is a recommended alternative for patients with primary mitral regurgitation who are inoperable or at high surgical risk—supported by Class IIa, Level of Evidence (LoE) B. Early intervention is key, even in asymptomatic cases, especially when signs of cardiac damage like tricuspid regurgitation or left atrial enlargement are present.
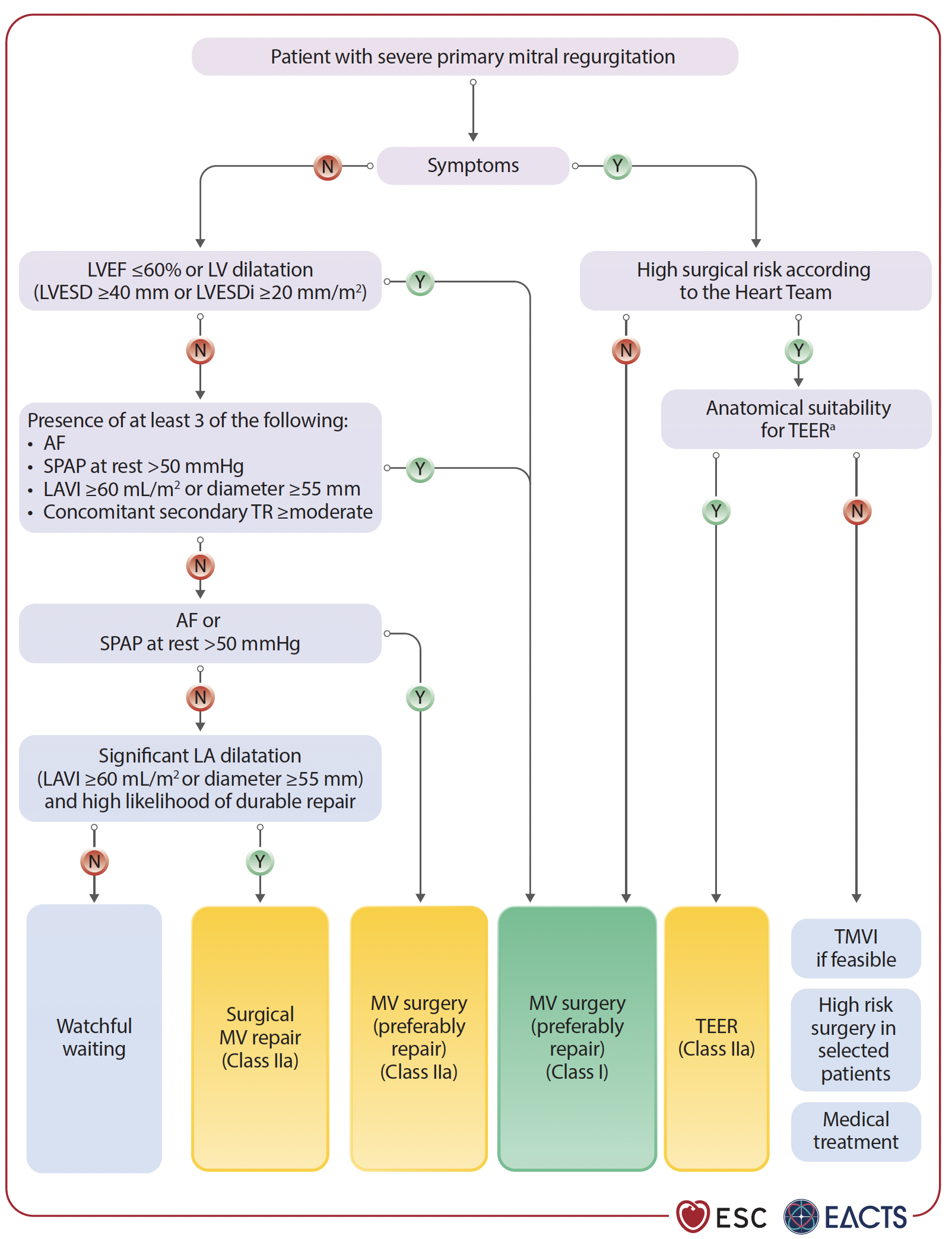
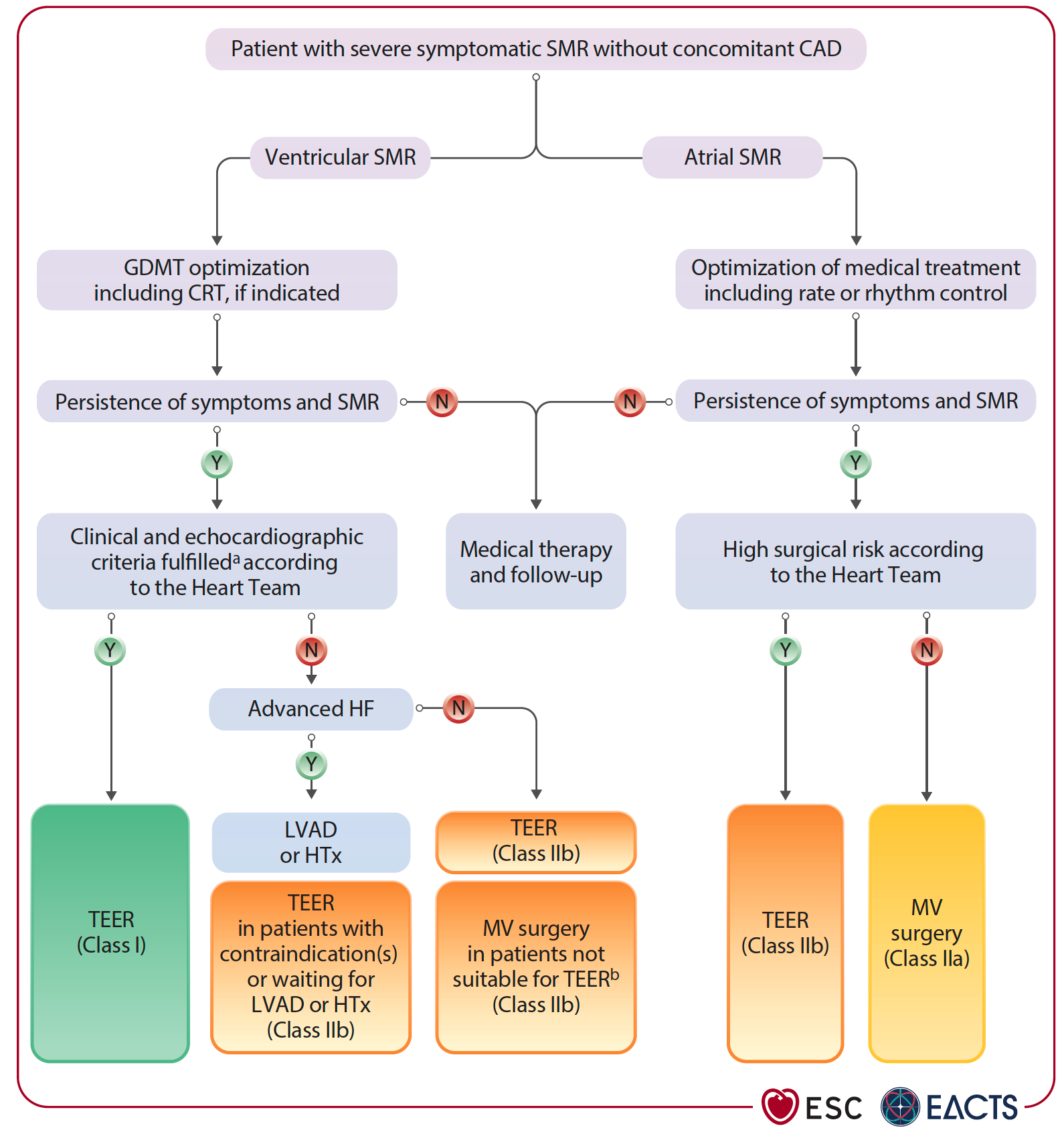
TEER is a Class I, LoE A recommendation for patients with ventricular SMR who remain symptomatic despite optimal medical treatment. In atrial SMR, surgery combined with AF ablation and LAAO may help, especially in patients with persistent symptoms and high stroke risk. TEER is also an option for those unsuitable for surgery, supported by a Class IIb, LoE B recommendation.
The approach to mitral stenosis (MS) is evolving. Rheumatic MS is still treated with percutaneous mitral commissurotomy when anatomy allows, while surgery is reserved for complex cases. For degenerative MS linked to mitral annular calcification, guidelines now support transcatheter mitral valve implantation (TMVI) in select patients—reflecting growing expertise in this challenging area. TMVI has been deemed as Class IIb, LoE C.
| PMR | SMR |
|---|---|
| Esc/eacts – Guidelines for the management of Valvular Heart Disease (2021)16 | |
Evaluation
| Evaluation
|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF PATIENTS WITH VALVULAR HEART DISEASE (2020)22 | |
Initial diagnosis
Changing signs or symptoms
Routine follow-up
Exercise testing
| Diagnosis
|
| PMR | SMR |
|---|---|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE (2022)28 | |
N/A |
|
| ESC/EACTS – GUIDELINES FOR THE MANAGEMENT OF VALVULAR HEART DISEASE (2021)16 | |
In acute MR:
|
|
| HFA/EACVI/EHRA/EAPCI/ESC JOINT POSITION STATEMENT ON THE MANAGEMENT OF SMR (2021) | |
N/A |
|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF PATIENTS WITH VALVULAR HEART DISEASE (2020)22 | |
|
|
| PMR | SMR |
|---|---|
| ACC/AHA – GUIDELINE FOR THE MANAGEMENT OF HEART FAILURE (2022)28 | |
N/A |
|
| ESC/EACTS – GUIDELINES ON THE MANAGEMENT OF VALVULAR HEART DISEASE (2021)16 | |
|
|
| ESC – GUIDELINES FOR THE DIAGNOSIS AND TREATMENT OF ACUTE AND CHRONIC HF (2021)15 | |
N/A |
|
| HFA/EACVI/EHRA/EAPCI/ESC JOINT POSITION STATEMENT ON THE MANAGEMENT OF SMR IN PATIENTS WITH HF (2021)29 | |
N/A |
|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF PATIENTS WITH VALVULAR HEART DISEASE (2020)22 | |
|
|
| PMR | SMR |
|---|---|
| ACC/AHA – GUIDELINE FOR THE MANAGEMENT OF HEART FAILURE (2022)28 | |
N/A |
|
| ESC/EACTS – GUIDELINES FOR THE MANAGEMENT OF VALVULAR HEART DISEASE (2021)16 | |
|
|
| ESC – GUIDELINES FOR THE DIAGNOSIS AND TREATMENT OF ACUTE AND CHRONIC HF (2021)15 | |
N/A |
|
| HFA/EACVI/EHRA/EAPCI/ESC JOINT POSITION STATEMENT ON THE MANAGEMENT OF SMR IN PATIENTS WITH HF (2021)29 | |
N/A |
|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF PATIENTS WITH VALVULAR HEART DISEASE (2020)22 | |
|
|
| PMR | SMR |
|---|---|
| ESC/EACTS – GUIDELINES FOR THE MANAGEMENT OF VALVULAR HEART DISEASE (2021)16 | |
N/A |
|
| ESC GUIDELINES FOR THE DIAGNOSIS AND TREATMENT OF ACUTE AND CHRONIC HF (2021)15 | |
N/A |
|
| ACC/AHA – GUIDELINES FOR THE MANAGEMENT OF PATIENTS WITH VALVULAR HEART DISEASE (2020)22 | |
|
|